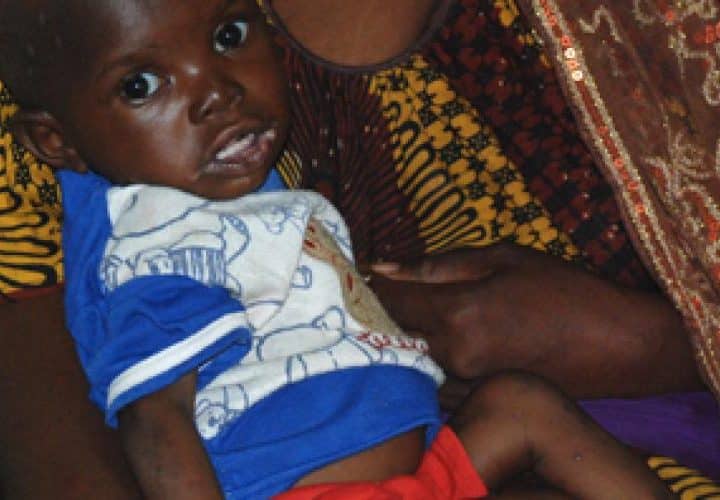
Malnutrition remains a critical public health challenge in Mali, affecting millions across this West African nation of 15 million people. Despite ongoing prevention efforts, pockets of severe nutritional deficits persist across the country.
Mali faces significant malnutrition challenges with nearly 1 in 5 Malian children dying before age five, highlighting the urgent need for sustained intervention. This silent crisis impacts families and the nation’s future, with consequences spanning short, medium, and long-term health outcomes.
In many Malian households, closely spaced pregnancies contribute to high malnutrition rates among young children and mothers. Larger family sizes correlate with increased malnutrition incidence, creating a vicious cycle of poverty and poor health.
Critical malnutrition rates exceed global thresholds
Acute malnutrition affects 15% of Mali’s population, surpassing the World Health Organization’s 10% alert threshold. Chronic malnutrition impacts 38% of children under five—nearly double the 20% international alert level. Mali’s iron deficiency rates are among the world’s highest, with over 80% of children under five and 65% of women affected.
A severe iron deficiency impairs children’s intellectual development and learning capacity. For mothers, iron deficiency during pregnancy increases risks of delivering malnourished infants. With 40% of Mali’s population affected, this nutritional crisis demands immediate attention.
Strategic interventions to combat malnutrition
The Malian government has implemented a comprehensive nutrition policy with targeted action plans to improve prevention and treatment services.
“This strategy includes mobilizing sector-specific funding to strengthen our nutritional response capabilities”
The government recently mandated universal salt iodization, now reaching 79% of households—though still below the 90% target. Since 2005, bi-annual intensified nutrition weeks have covered 95% of the country, focusing on children aged 6-59 months.
These community-driven initiatives have become integral to local health practices. During these campaigns, health workers promote vitamin A supplementation and deworming tablets, significantly reducing child mortality rates. The UNICEF-supported approach empowers communities to identify malnutrition signs, detect cases early, and provide timely interventions.
By 2010, 50% of severely malnourished children received treatment, with coverage gradually increasing as awareness and healthcare access improve.